“40% of American adults will develop type 2 diabetes in their lifetime”—CDC study shows.
This horrendous statistic shows the rise of our relentless plague of modern diseases; diabetes, overweight, cardiovascular disease, stroke and Alzheimer’s (now thought to have a common cause—the latter being reclassified as diabetes type 3). As the authors of the study that produced this frightening statistic conclude, “These findings…emphasize the need for effective interventions to reduce incidence.”
The search for “effective interventions” has been a long one and with few real results; only band-aid solutions. Our western dietis killing us, even though studies show that Americans do their best to follow the ever–changing dietary guidelines, and yet the plague keeps progressing; claiming ever more victims. A recent profile in the Wall Street Journal outlined a new diet approach that shows promise:
“Until now, most diets have been based on the glycemic index, a half-century-old list that ranks foods based on how they affect blood sugar. While this index is widely used by doctors to provide dietary advice, it is based on an average response and has been found wanting because many people aren’t average.”
—Dietary Advice Based on the Bacteria in Your Gut, Charles Wallace, WSJ.com, Feb 25, 2018 10:05 p.m. ET
This new approach came out of research done by the Weizmann Institute of Science, Israel (their results were published HEREin the scientific journal, Cell). Their study showed that many factors determine the glycemic response (how quickly food turns to sugar in the blood stream) but that the main factor is the variation in the composition and population of bacteria in the gut (the 100 trillion bacteria, viruses and fungi cells that inhabit the human digestive tract).
Through continuous monitoring of the Blood Glucose (BG) levels of some 800 test subjects, they discovered that the glycemic response was very different in a large number of individuals for the same foods. For example, some people had a large BG spike for rice, some had moderate spikes and some had no spike at all.
My wife and I set out to test the hypothesis with an informal experiment. We both consumed 100g of parboiled white rice with butter and pecorino cheese. Something approximate to this Glycemic Index entry:

The glycemic data above was the average from 15 test subjects over a period of 4 hours. According to the numbers, it should not have created a BG spike (GI) nor raised our BG for very long (GL). These were our results (testing every 30 minutes):
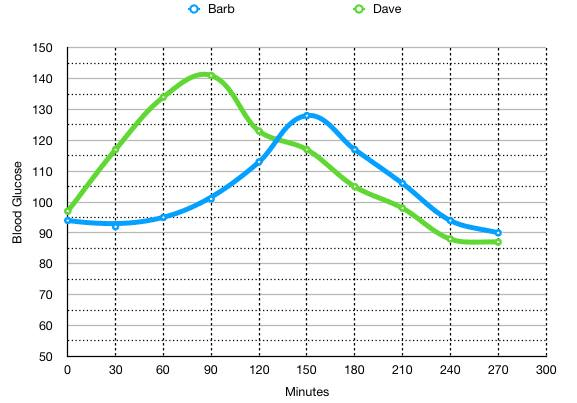
Just as a comment about the experience, I felt great the whole time, but on the backside of the curve, I started to get hungry (like many people do after carbohydrates). But, this was a “false” hunger, as I clearly had enough blood sugar. I started at 96 but at the end “crashed” at 88 where I was then, very hungry.
My wife on the other hand is not a typical consumer of carbohydrates (she strips the breading off of shrimp, for example). She felt like she was, “punched in the stomach” the whole time. As the graph shows, her system did not readily convert the starch in the rice to sugar. Her response was delayed and moderate, while I had a spike, followed by a long decline (where insulin is converting most of the sugar to fat).
According to the study, the difference in our reactions is due to the differences in our respective gut bacteria (microbiome). This difference, according to the authors Dr. Eran Segal and Dr. Eran Elinav, is why I am overweight and my wife is not. My microbiome is very efficient at converting the starch in rice to body fat, while hers is not. All because the bacteria that live in our digestive tracts are different.
Segal and Elinav developed a machine-learning algorithm that analyzed the microbiome DNA and blood test data of the subjects in a subsequent study to try and predict how a subject’s BG levels would respond to certain foods. That way their software could recommend a “good” diet or a “bad” diet (see chart B below). The results were confirmed and the system was able to provide diet choices that would or would not cause a glucose spike. They licensed the technology to a startup called, DayTwonow a leader in personalizednutrition (mentioned in the WSJ article quoted above).
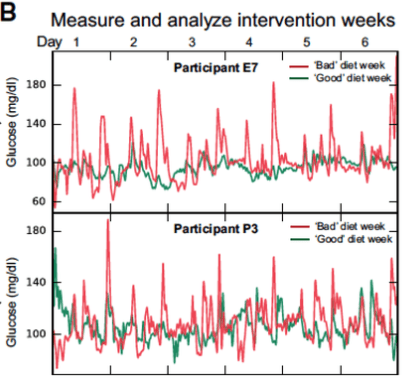
Goodand Baddiet BG results from the study.(View the TED talk on YouTube)
This personalized model and its potential was not lost on SAP co-founder, Hasso Platner after the inception of HANA (an in-memory columnar database). Such innovations have enabled such agile solutions to be tailored to specific conditions (like a patient’s unique microbiome) and opened up new levels of patient care never before possible.
“Trends such as personalized medicine and new medical technologies will change the way diseases are diagnosed and treated. In this operating model, medical decisions, such as therapy approaches to be applied and drugs to be used, are tailored specifically to the individual conditions of the patient.“
—“The In-Memory Revolution: How SAP HANA Enables Business of the Future,” Hasso Platner & Bernd Leukert, Springer Int. Pub., Switzerland 2015, page 158
Back in the early days of modern western medicine, the practice was highly personalized, doctors made house calls almost exclusively, and the patient dictated the course of treatment. After the Enlightenment that all changed and medicine became more “clinical” and impersonal. This digital transformation is making the transition back to personalized health, medical advice and treatment possible. The potential of this personalized approach to health and medicine is just being tapped. Perhaps we are looking at the begining of the end of our current plague and the start of a new era of customized and effective intervention.




